Centrally Acting Sympatholytics
General Pharmacology
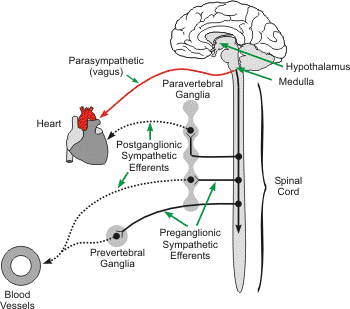 The sympathetic adrenergic nervous system plays a major role in regulating arterial pressure. Activation of these nerves to the heart increases the heart rate (positive chronotropy), contractility (positive inotropy) and velocity of electrical impulse conduction (positive dromotropy). The norepinephrine-releasing, sympathetic adrenergic nerves that innervate the heart and blood vessels are postganglionic efferent nerves whose cell bodies originate in prevertebral and paravertebral sympathetic ganglia. Preganglionic sympathetic fibers, which travel from the spinal cord to the ganglia, originate in the medulla of the brainstem. Within the medulla are located sympathetic excitatory neurons that have significant basal activity, which generates a level of sympathetic tone to the heart and vasculature, even under basal conditions. The sympathetic neurons within the medulla receive input from other neurons within the medulla (e.g., vagal neurons), from the nucleus tractus solitarius (receives input from peripheral baroreceptors and chemoreceptors), and from neurons in the hypothalamus. Together, these neuronal systems regulate sympathetic (and parasympathetic) outflow to the heart and vasculature.
The sympathetic adrenergic nervous system plays a major role in regulating arterial pressure. Activation of these nerves to the heart increases the heart rate (positive chronotropy), contractility (positive inotropy) and velocity of electrical impulse conduction (positive dromotropy). The norepinephrine-releasing, sympathetic adrenergic nerves that innervate the heart and blood vessels are postganglionic efferent nerves whose cell bodies originate in prevertebral and paravertebral sympathetic ganglia. Preganglionic sympathetic fibers, which travel from the spinal cord to the ganglia, originate in the medulla of the brainstem. Within the medulla are located sympathetic excitatory neurons that have significant basal activity, which generates a level of sympathetic tone to the heart and vasculature, even under basal conditions. The sympathetic neurons within the medulla receive input from other neurons within the medulla (e.g., vagal neurons), from the nucleus tractus solitarius (receives input from peripheral baroreceptors and chemoreceptors), and from neurons in the hypothalamus. Together, these neuronal systems regulate sympathetic (and parasympathetic) outflow to the heart and vasculature.
Sympatholytic drugs can block this sympathetic adrenergic system are three different levels. First, peripheral sympatholytic drugs such as alpha-adrenoceptor and beta-adrenoceptor antagonists block the influence of norepinephrine at the effector organ (heart or blood vessel). Second, there are ganglionic blockers that block impulse transmission at the sympathetic ganglia. Third, there are drugs that block sympathetic activity within the brain. These are called centrally acting sympatholytic drugs.
Centrally acting sympatholytic drugs block sympathetic activity by binding to and activating postjunctional alpha2 (α2)-adrenoceptors or imidazoline type 1 (I1) receptors found in the central nervous system, particularly in the rostral ventrolateral medulla and nucleus tractus solitarius. This reduces sympathetic outflow to the heart, decreasing cardiac output by decreasing heart rate and contractility. Reduced sympathetic output to the vasculature decreases sympathetic vascular tone, which causes vasodilation and reduced systemic vascular resistance, which decreases arterial pressure.
Therapeutic Indications
Centrally acting α2-adrenoceptor agonists are used in the treatment of hypertension. However, they are not considered first-line therapy because of side effects that are associated with their actions within the brain. They are usually administered in combination with a diuretic to prevent fluid accumulation, which increases blood volume and compromises the blood pressure lowering effect of the drugs. Fluid accumulation can also lead to edema. Centrally acting α2-adrenoceptor agonists are effective in hypertensive patients with renal disease because they do not compromise renal function.
Specific Drugs
Several centrally acting α2-adrenoceptor/imidazoline I1 agonists are available for clinical use:
- clonidine
- guanabenz
- guanfacine
- methyldopa
- moxonidine
- rilmenidine
Clonidine, guanabenz and guanfacine are structurally related compounds and have similar antihypertensive profiles. α-methyldopa is a structural analog of dopa and functions as a prodrug. After administration, α-methyldopa is converted to α-methylnorepinephrine, which then serves as the α2-adrenoceptor agonist in the medulla to decrease sympathetic outflow.
Clonidine, when given intravenously, causes initial vasoconstriction via vascular α2-adrenoceptors; however, this changes to vasodilation as the clonidine binds to α2-adrenoceptors in the central nervous system, which decreases sympathetic efferent activity and lowers blood pressure. The oral form does not display initial vasoconstriction. Clonidine may also inhibit norepinephrine release by sympathetic nerves that innervate blood vessels, thus offsetting the constrictor effects on vascular smooth muscle postjunctional receptors. Central stimulation by clonidine also increases parasympathetic outflow, which can reduce heart rate. Guanabenz, guanfacine and methyldopa have actions that are like clonidine.
Moxonidine and rilmenidine are relatively selective for I1-imidazoline receptors.
Side Effects and Contraindications
Side effects of centrally acting α2-adrenoceptor agonists include sedation, dry mouth and nasal mucosa, bradycardia (because of increased vagal stimulation of the SA node and sympathetic withdrawal), orthostatic hypotension, and impotence. Constipation, nausea and gastric upset are also associated with the sympatholytic effects of these drugs. Fluid retention and edema are also a problem with chronic therapy; therefore, concurrent therapy with a diuretic is necessary. Sudden discontinuation of clonidine can lead to rebound hypertension, which results from excessive sympathetic activity.
Side effects are less prominent for the imidazoline agonists.
Revised 04/27/2024

 Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021)
Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021) Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)
Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)