Autonomic Nervous System
The autonomic nervous system (ANS) can be thought of as an "automatic" neural control system that the body uses to regulate organ function. The ANS is involuntary in that a person cannot normally exert conscious control over its function. For example, although the ANS plays an important role in regulating the heart rate, a person at rest cannot normally increase or decrease the heart rate by conscious will in the same way that one can decide to raise an arm or speak.
The ANS has two basic divisions — sympathetic and parasympathetic. These divisions have opposite effects and usually work reciprocally. For example, the sympathetic branch of the ANS, when activated, increases the heart rate, whereas activation of the parasympathetic branch reduces the heart rate.
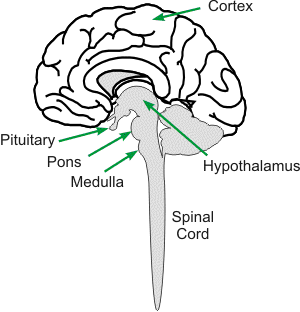 The ANS originates just above the spinal cord in a region of the lower brain (brainstem) called the medulla oblongata. Within the medulla are nerve cell bodies that fire action potentials and generate autonomic nerve activity. Some of these cell bodies are grouped together into distinct locations called nuclei. The nucleus ambiguous (NA), for example, contains cell bodies of parasympathetic vagus nerves (tenth cranial nerves) that send axons out to the body through the vagus nerves to innervate the heart and other visceral organs. Other cells in the medulla make up the cell bodies that regulate sympathetic activity. These cells are not tightly grouped into nuclei, although there are distinct medullary regions that have high populations of these cells. Two important regions controlling sympathetic activity are the rostral ventrolateral medulla (RVLM) and caudal ventrolateral medulla (CVLM). Sympathetic neurons in the RVLM are spontaneously active and are modulated by interneuronal fibers from the CVLM and nucleus ambiguus. Axons from the RVLM travel down the spinal cord, synapse within the intermediolateral horn of the spinal cord, then exit the spinal cord as preganglionic efferent sympathetic nerves to innervate the heart, blood vessels, and other organs. The vagal nerve fibers that leave the medulla are referred to as preganglionic vagal efferent nerves because they travel away from their origin in the brainstem to synapse within distal ganglia. Click here to learn more about efferent autonomic nerves and autonomic ganglia.
The ANS originates just above the spinal cord in a region of the lower brain (brainstem) called the medulla oblongata. Within the medulla are nerve cell bodies that fire action potentials and generate autonomic nerve activity. Some of these cell bodies are grouped together into distinct locations called nuclei. The nucleus ambiguous (NA), for example, contains cell bodies of parasympathetic vagus nerves (tenth cranial nerves) that send axons out to the body through the vagus nerves to innervate the heart and other visceral organs. Other cells in the medulla make up the cell bodies that regulate sympathetic activity. These cells are not tightly grouped into nuclei, although there are distinct medullary regions that have high populations of these cells. Two important regions controlling sympathetic activity are the rostral ventrolateral medulla (RVLM) and caudal ventrolateral medulla (CVLM). Sympathetic neurons in the RVLM are spontaneously active and are modulated by interneuronal fibers from the CVLM and nucleus ambiguus. Axons from the RVLM travel down the spinal cord, synapse within the intermediolateral horn of the spinal cord, then exit the spinal cord as preganglionic efferent sympathetic nerves to innervate the heart, blood vessels, and other organs. The vagal nerve fibers that leave the medulla are referred to as preganglionic vagal efferent nerves because they travel away from their origin in the brainstem to synapse within distal ganglia. Click here to learn more about efferent autonomic nerves and autonomic ganglia.
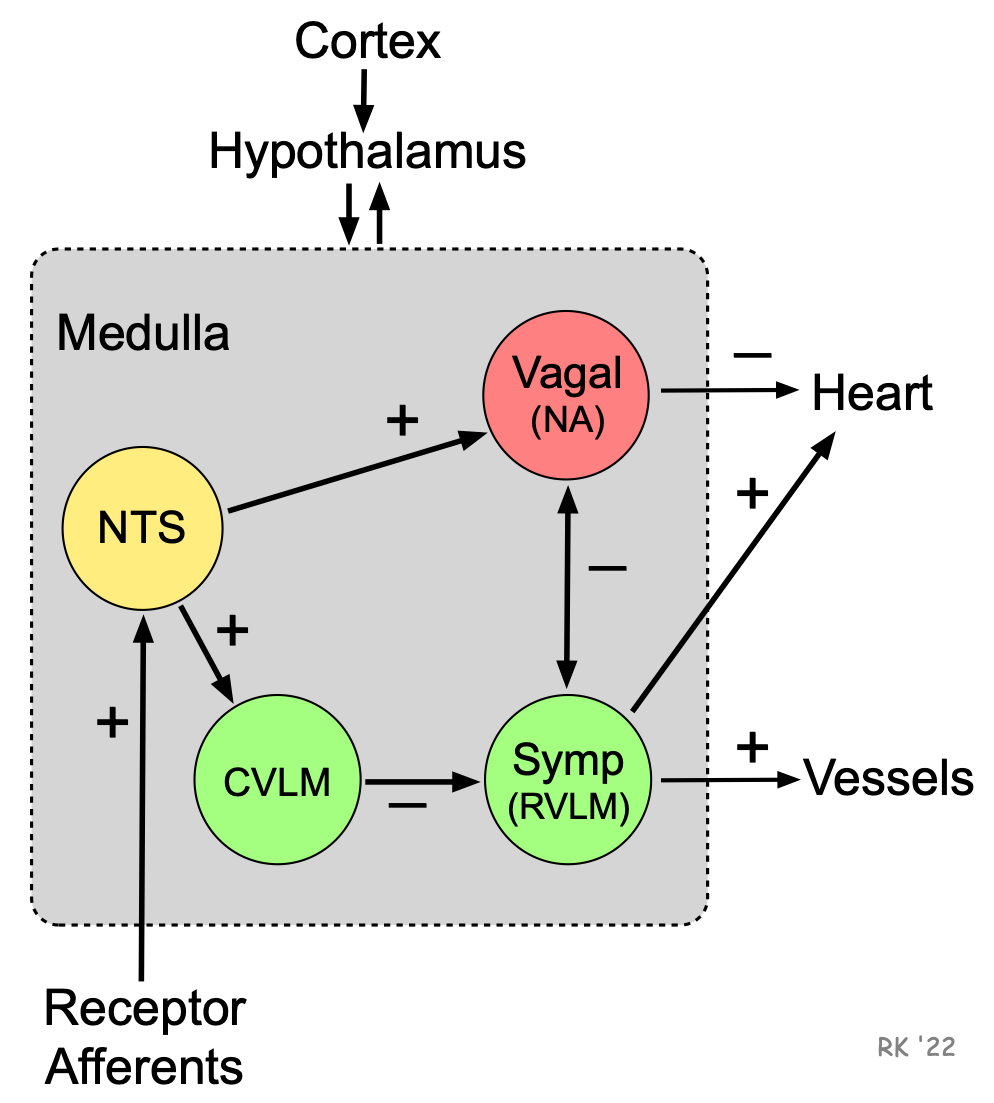 The spontaneous activity of autonomic nerves is regulated by different sensory receptors in the body that monitor physiological function. These sensory receptors generate action potentials in response to changes in mechanical, chemical and thermal stimuli. The action potentials are conducted to the medulla via afferent nerves. Sensory receptors that are involved in regulating blood pressure are called baroreceptors, a type of mechanoreceptor. These receptors respond to stretching of the walls of blood vessels or cardiac chambers. This increases the firing of these receptors, which then send this information via conducted action potentials up to the nucleus tractus solitarius (NTS) of the medulla. Increased activity of the NTS stimulates parasympathetic (vagal) activity and decreases sympathetic activity within the medulla through interneuronal projections. There are also connections between the vagal and sympathetic neurons that cause reciprocal inactivation. In this way, regions in the medulla that control autonomic outflow receive information on blood pressures within different regions of the cardiovascular system.
The spontaneous activity of autonomic nerves is regulated by different sensory receptors in the body that monitor physiological function. These sensory receptors generate action potentials in response to changes in mechanical, chemical and thermal stimuli. The action potentials are conducted to the medulla via afferent nerves. Sensory receptors that are involved in regulating blood pressure are called baroreceptors, a type of mechanoreceptor. These receptors respond to stretching of the walls of blood vessels or cardiac chambers. This increases the firing of these receptors, which then send this information via conducted action potentials up to the nucleus tractus solitarius (NTS) of the medulla. Increased activity of the NTS stimulates parasympathetic (vagal) activity and decreases sympathetic activity within the medulla through interneuronal projections. There are also connections between the vagal and sympathetic neurons that cause reciprocal inactivation. In this way, regions in the medulla that control autonomic outflow receive information on blood pressures within different regions of the cardiovascular system.
The autonomic regions of the medulla also receive input from the hypothalamus that is located at the base of the brain. Special regions within the hypothalamus are involved in integrating cardiovascular responses to exercise and thermal stress, for example. When a person exercises, coordinated changes must occur in cardiac and vascular function, which is the role of the hypothalamus. For example, electrical stimulation of specific regions in the hypothalamus can elicit cardiovascular changes (e.g., increased heart rate and blood pressure) in an anesthetized animal that closely mimics what occurs during flight-or-fright responses.
Brain regions above the hypothalamus, such as the cortex, can also influence medullary centers. For example, fear and anxiety can lead to increases in blood pressure and heart rate through activation of the sympathetic nervous system.
Revised 11/29/2023

 Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021)
Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021) Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)
Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)