Autonomic Ganglia
Anatomy
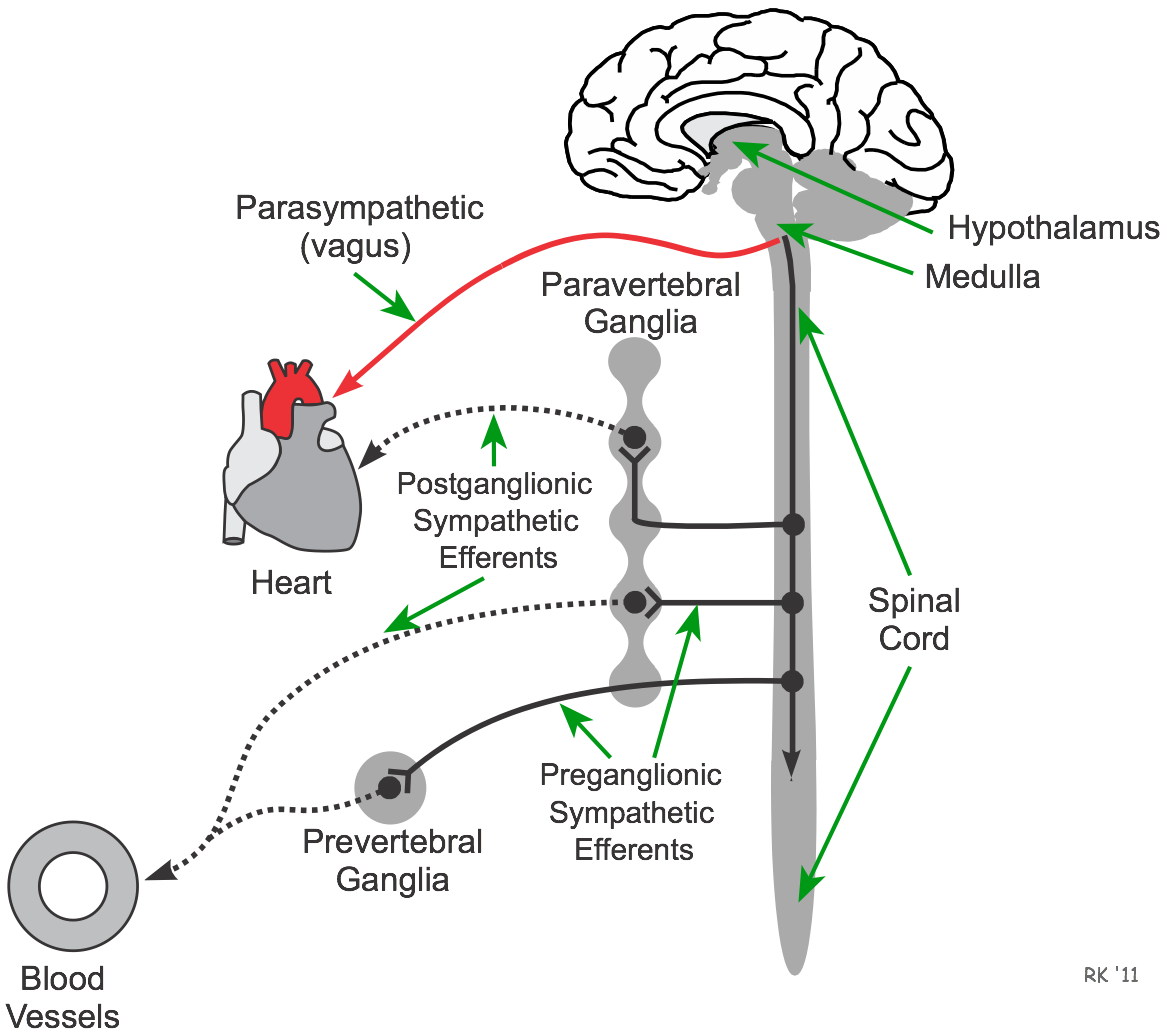 The autonomic nervous system plays a major role in regulating cardiac and vascular function. Parasympathetic (vagal) nerves leave the vagal nuclei within the medulla as preganglionic efferent vagal fibers. These preganglionic efferent fibers are relatively long and do not synapse until they reach their target organ (e.g., the heart). The preganglionic fibers synapse within small ganglia near the target tissue (e.g., the sinoatrial node), where they release the neurotransmitter acetylcholine (ACh). ACh binds to nicotinic receptors, causing depolarization and action potential generation in the short postganglionic vagal fibers that synapse at the target cells (see figure). The neurotransmitter released by these postganglionic fibers at the target tissue is also ACh, and it binds to muscarinic receptors.
The autonomic nervous system plays a major role in regulating cardiac and vascular function. Parasympathetic (vagal) nerves leave the vagal nuclei within the medulla as preganglionic efferent vagal fibers. These preganglionic efferent fibers are relatively long and do not synapse until they reach their target organ (e.g., the heart). The preganglionic fibers synapse within small ganglia near the target tissue (e.g., the sinoatrial node), where they release the neurotransmitter acetylcholine (ACh). ACh binds to nicotinic receptors, causing depolarization and action potential generation in the short postganglionic vagal fibers that synapse at the target cells (see figure). The neurotransmitter released by these postganglionic fibers at the target tissue is also ACh, and it binds to muscarinic receptors.
Sympathetic nerves that originate within the medulla travel down the spinal cord, where they synapse with preganglionic cell bodies within the spinal cord. These cell bodies give off preganglionic fibers that are relatively short (compared to the long preganglionic vagal efferent fibers). These preganglionic fibers enter the paravertebral ganglia (sympathetic chain ganglia) that are found on either side of the spinal column. Either at the same level they enter the chain ganglia, or after traveling up or down the chain, these preganglionic neurons synapse with the cell bodies of postganglionic sympathetic fibers. ACh is the neurotransmitter within these ganglia, and the ACh binds to nicotinic receptors on postganglionic neurons (see figure). From these neurons arise relatively long postganglionic fibers that travel to their target organ and release norepinephrine as the primary neurotransmitter, which binds to alpha- or beta-adrenoceptors on the target tissue.
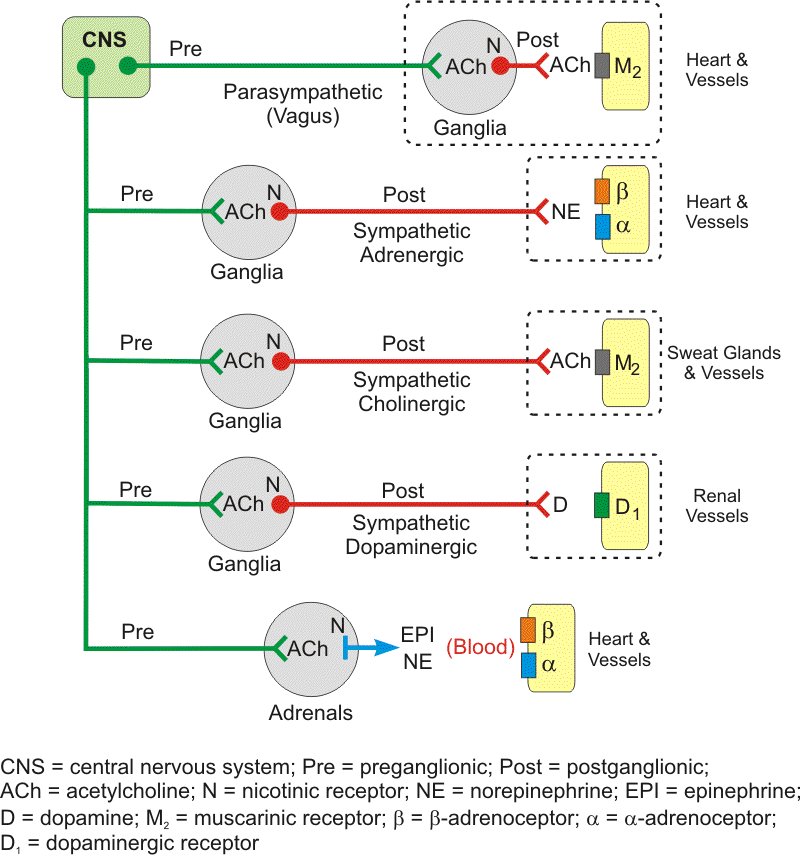 Some preganglionic sympathetic fibers, instead of synapsing within paravertebral ganglia, synapse in prevertebral ganglia within the abdomen (celiac, superior mesenteric, and inferior mesenteric ganglia). ACh, which binds to nicotinic receptors, is the neurotransmitter at these sites as found in the other autonomic ganglia. Postganglionic sympathetic fibers then travel from the prevertebral ganglia to innervate tissues such as blood vessels where they release norepinephrine as the primary neurotransmitter, which binds primarily to vascular alpha-adrenoceptors. Therefore, sympathetic postganglionic fibers can originate in either paravertebral or prevertebral ganglia.
Some preganglionic sympathetic fibers, instead of synapsing within paravertebral ganglia, synapse in prevertebral ganglia within the abdomen (celiac, superior mesenteric, and inferior mesenteric ganglia). ACh, which binds to nicotinic receptors, is the neurotransmitter at these sites as found in the other autonomic ganglia. Postganglionic sympathetic fibers then travel from the prevertebral ganglia to innervate tissues such as blood vessels where they release norepinephrine as the primary neurotransmitter, which binds primarily to vascular alpha-adrenoceptors. Therefore, sympathetic postganglionic fibers can originate in either paravertebral or prevertebral ganglia.
The second figure additionally shows the existence of postganglionic sympathetic cholinergic fibers that innervate sweat glands and vessels. The sympathetic cholinergic postganglionic nerves release ACh, which binds to muscarinic receptors. Sympathetic cholinergic nerves also innervate skeletal muscle arteries in some species (dogs and cats, but not humans). There are also postganglionic sympathetic dopaminergic nerves that release dopamine, which binds to dopaminergic receptors in the kidneys. Finally, preganglionic sympathetic nerves to the adrenal medulla glands release ACh that stimulates the production and release of catecholamines (epinephrine primarily, norepinephrine secondarily).
Physiology
Activation of sympathetic adrenergic nerves to the heart releases norepinephrine that binds to adrenergic receptors (primarily beta-adrenoceptors), which increases heart rate (positive chronotropy), contractility (positive inotropy) and velocity of electrical impulse conduction (positive dromotropy). Together, these changes increase cardiac output and arterial blood pressure. Sympathetic adrenergic activation also constricts blood vessels through the actions of norepinephrine binding to alpha-adrenoceptors. This increases arterial blood pressure. In contrast, activation of vagal efferent nerves depresses heart function through the effects of ACh binding to muscarinic receptors. Except for a few specific organs, there is little or no vagal innervation of blood vessels. Therefore, the cardiovascular effects of vagal activation are primarily mediated through the heart, whereas sympathetic activation affects both the heart and vasculature. Sympathetic cholinergic activation releases ACh that binds to muscarinic receptors, which stimulates sweating and dilates arteries in the skin. Activation of sympathetic cholinergic nerves to skeletal muscle arteries during exercise or the "defense reaction" causes vasodilation in some species. Sympathetic dopaminergic activation to the kidneys dilates renal vessels through dopamine binding to dopaminergic receptors. This increases renal blood flow and renal glomerular filtration. Finally, the preganglionic sympathetic nerves that synapse in the adrenal glands stimulate catecholamine release that circulates in the blood to impact the heart, blood vessels and other organs by binding to adrenergic receptors.
It is important to note that under basal, resting conditions, vagal and sympathetic adrenergic nerves are tonically active. In the heart because vagal influences override sympathetic effects, there is a resting vagal tone that maintains a low-resting heart rate. In contrast, most blood vessels, which have little or no vagal innervation, are dominated by sympathetic adrenergic influences at rest, giving rise to what is termed "sympathetic vascular tone." Therefore, blocking ganglionic neurotransmission by a ganglionic blocker removes vagal tone on the heart and sympathetic vascular tone.
Revised 11/29/2023

 Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021)
Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021) Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)
Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)